Lupus is an autoimmune disease which can lead to inflammation and damage to the skin, joints, brain, kidneys, and other organs, and is one of the more dangerous categories of autoimmune disease.
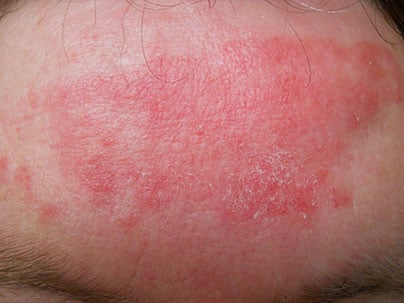
It is unclear what the actual prevalence of lupus is, but it has been estimated that in the U.S. it is approximately 161,000 to 322,000, or 0.1% of the population.1 Most of those diagnosed with lupus are young women.
Common symptoms of lupus may include:
If lupus goes uncontrolled, severe consequences can occur including organ damage and death. Persons with lupus have a higher risk of blood clots, kidney failure, heart disease, and stroke.
Little is known about what exactly causes lupus in individuals, but investigators believe it is a combination of genetic and environmental factors such as diet, toxin exposures, and intestinal bacteria imbalance.
Dr. Fuhrman’s general supplement protocol for adults (see Vitamin Advisor for details) includes:
Multivitamin (without beta-carotene, vitamin A, vitamin E, folic acid, copper), such as Women’s Daily Formula +D3, Men’s Daily Formula +D3, or Gentle Care Formula.
Omega-3 DHA and EPA, such as DHA+EPA Purity.
Optional: Consider adding a mixed mushroom immune supplement, such as Immune Biotect, because of the potential immune system benefits throughout life from assorted mushroom phytochemicals not normally consumed in the diet. Consult your physician if you are on medication.
For supplement recommendations personalized to you, your health condition and goals, visit the Personalized Vitamin Advisor and answer a few questions.
Sign up for the online Combat Autoimmune Disease and Cancer Masterclass
Supervised, periodic water fasting can be used as an adjunct treatment for autoimmune conditions. I have documented remission of autoimmune diseases following supervised fasting in a published series of case reports.29 Additional studies have found that fasting (followed by a vegetarian diet) reduces pain in rheumatoid arthritis patients.30, 31 Continuing to follow a Nutritarian diet after completing the fast is essential for sustaining the benefits of the fast. Fasting puts the body into a repair mode, facilitating the elimination of damaged molecules, reducing inflammation, and resetting the immune system.32, 33
ONLINE: All members of DrFuhrman.com can search the Ask the Doctor archives for discussions on this topic. Platinum and Diamond members can connect with Dr. Fuhrman by posting questions in the forum. Not a member? Join now.
IN PERSON or ONLINE: Book a consultation with a specialist at Longevity Rx in San Diego, California, run by Joel Fuhrman, MD and Cara Fuhrman, ND. Using nutritional protocols, cutting-edge screening tools, advanced imaging, and innovative treatments for pain and injuries, they'll create a personalized action plan to help you prevent and recover from illness, and achieve your optimal weight. Book online at Longevity Rx or call +1 (858) 367-3558
EVENTS: Join Dr. Fuhrman for an online boot camp, detox or other event. During these immersive online events, you’ll attend zoom lectures, follow a special meal plan, and have access to a special, live Q&A session with Dr. Fuhrman. Learn more about events.
The following are sample questions from the Ask the Doctor Community Platinum and higher members can post their health questions directly to Dr. Fuhrman. (All members can browse questions and answers.)
For someone who has lupus nephritis, what are the food restrictions? I heard that a certain amount of protein can damage the kidneys even more. Are there foods that can help the kidneys? Thanks.
Did you read my book, Super Immunity? The diet and supplement protocol in the book is what I want you to do. The main point for lupus nephritis is no animal products, salt or oil, in other words, a strict vegan diet. You can eat brown and wild rice and vegetables, mushrooms, squash, and greens, with a small amount of fruit and a limited amount of nuts, seeds, and beans to keep protein fairly low. You can eat a half cup of beans with each meal, you can eat one ounce of seeds and nuts with each meal, and you can eat up to two fresh fruits with each meal. You should not have animal products at all until you are better.
I have been following your autoimmune protocol for lupus nephritis for a little over a month now, and I still don’t see any improvement. When should I start feeling better and have no more protein in the urine? I also eliminated wheat, oil, and salt. Will I ever be able to eat any type of animal product in the future?
It takes at least 3 months to get the micronutrient load built up in your tissues, but it might take even longer to see results. Your immune system and disease process can’t just reverse itself in a few weeks. Your condition is serious enough that you should avoid animal products for a long time now, until we see things are significantly improved.
I have seen some very severely ill patients with this condition get well. I often begin to see improvement after the first 3-4 months, but I have seen lupus patients take a few years to get well, making slow progress.

Sharon lost 42 pounds; her lupus numbers are in normal range and she has more engergy than ever... Read More
Results may vary.
Suffering the debilitating effects of lupus and multiple autoimmune diseases made Lynsey's life miserable; now with her 65 pound weight loss her life has a new vibrancy... Read More
Results may vary.