Cholesterol is one type of lipid or fat in the body. It is synthesized predominately in the liver and used to make steroid hormones and is required for bile acid which aids in digestion and absorption of dietary fats. Cholesterol is also found in our diet, with a vast majority consumed from animal products. When animal products and processed foods rich in saturated and trans fats are consumed in excess amounts, high cholesterol, along with the inflammation produced from eating a low nutrient diet, will result in cholesterol plaques leading to cardiovascular disease.
An estimated 31.9 million adults (>/= 20 years of age) have a total serum cholesterol greater than 240, with a prevalence rate of 13.8%. The prevalence of abnormal lipids in youths ages 12 to 19 was 20.3%.1 As the dietary habits found in the Standard American Diet continue, prevalence rates will continue to increase among adults and children.
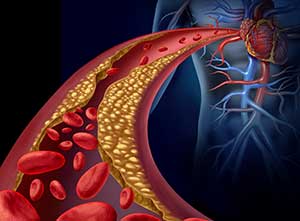
A cholesterol panel includes total cholesterol, LDL (low density lipoprotein), and HDL (high density lipoprotein) levels. LDL is referred to as “bad cholesterol” and HDL as “good cholesterol.” Cholesterol is packaged into lipoproteins when circulating in the blood; LDL carries cholesterol to the cells, and HDL delivers the excess back to the liver where it is broken down. Specialized lipid blood tests are able to evaluate the size and particle number of LDL. Having elevated numbers of small dense LDL particles increases CV risk. As these particles interact with and are degraded by white blood cells in an inflammatory environment that can arise from eating a SAD diet, foam cells form, and LDL can now easily accumulate as plaque build-up. Cholesterol plaque that covers the inner lining of arteries can cause obstruction and block blood flow to various organs. Ruptured cholesterol plaque can quickly form clots in arteries, leading to blockages.
Medications used to treat high cholesterol include those that stop the production of cholesterol in the liver or those that inhibit absorption of dietary cholesterol in the intestines. Statins like Lipitor and Crestor have been shown to increase the risk of myalgias, liver dysfunction, renal disease, macular degeneration, and diabetes.2 Not only is treating high cholesterol with a Nutritarian diet safer but it has been found to be even more effective at lowering LDL levels than medications.3
For supplement recommendations personalized to you, your health condition and goals, visit the Personalized Vitamin Advisor and answer a few questions.
Consuming a Nutritarian diet, which provides a substantial amount of plant sterols and stanols, works synergistically with exercise regimens to lower cholesterol levels. It changes the way cholesterol is absorbed, transported, and metabolized.6
* Foods containing at least 0.4 grams per serving of plant sterols, taken twice a day with meals for a daily total intake of at least 0.8 grams, as part of a diet low in saturated fat and cholesterol, may reduce the risk of heart disease. LDL Biotect provides 0.54 grams of plant sterols in each two-capsule serving.
ONLINE: All members of DrFuhrman.com can search the Ask the Doctor archives for discussions on this topic. Platinum and Diamond members can connect with Dr. Fuhrman by posting questions in the forum. Not a member? Join now.
IN PERSON: Book a stay at Dr. Fuhrman’s Eat to Live Retreat in San Diego, California. With options ranging from one, two and three months (and sometimes longer) you will be under Dr. Fuhrman’s direct medical supervision as you hit the “reset” button on your health. For more information: (949) 432-6295 or [email protected].
EVENTS: Join Dr. Fuhrman for an online boot camp, detox or other event. During these immersive online events, you’ll attend zoom lectures, follow a special meal plan, and have access to a special, live Q&A session with Dr. Fuhrman. Learn more about events.
The following are sample questions from the Ask the Doctor Community Platinum and higher members can post their health questions directly to Dr. Fuhrman. (All members can browse questions and answers.)
I work for a company where we have a significant financial incentive to score well on our BMI, cholesterol, and blood pressure. I have read several threads from those who are eating a Nutritarian diet, yet still scoring high on their blood tests, but you have stated that as long as they are eating predominantly high-nutrient foods and exercising, that high cholesterol number is not important. Then why do certain companies/doctors focus on these numbers?
I have followed a Nutritarian diet and practiced a very healthy lifestyle for years. I am at my optimal weight, (and have high cholesterol) so I will not be rewarded, however, my co-worker, who eats fast food but is on a statin, will!
I feel this encourages us to take the easy route (prescription drugs), rather than do what is best for our health (Nutritarian diet). Any comments? I have done everything you have suggested to bring my numbers down. My blood pressure is good, BMI great, triglycerides fine. Should I take a supplement?
I agree with you that a healthy diet with higher cholesterol is much healthier than a less healthy diet with lower cholesterol or medicated lower cholesterol. Plus, total cholesterol is not a good measurement of risk. One needs to consider the LDL particle number and size. The LDL particle size on a Nutritarian diet is much more favorable too, as are other markers demonstrating low inflammation. In conclusion, you are in phenomenal health, even if your LDL cholesterol does not drop below 100 as favored on those guidelines, whether it is recognized by your company’s standards or not.
After following a Nutritarian diet for several years now, I still struggle with less than ideal cholesterol. After the first year, my cholesterol went down below 200 (like 175). It has steadily crept up over the years. Last week, I had blood drawn for my annual physical and was shocked that the cholesterol number was 227. My LDL was 141. I’m 53, female, 5’7" and weigh 126 (this is my lowest weight in years).
My disappointment stems from me doubling my efforts to follow a Nutritarian diet. I have been making smoothies with spinach in the AM, salads for lunch, and salads and veggies for dinner. I have lost 5 pounds in the last 6 weeks alone!
One thing I have not done is keep up with my LDL protect supplements. I have not taken them for a few months. Could lack of the LDL Protect for a few months have caused such a difference when I am eating so well? Also, can stress cause a higher cholesterol level in the absence of bad eating? I recently lost my job.
Stopping the LDL and the increased stress can play a role, but most likely, this is caused by the recent weight loss and burning off more body fat (full of cholesterol). You must consider that you had plenty of stored saturated fats on your body that you autolysized, contributing to your continued utilization of those fats for cholesterol metabolism. In other words, you burned body fat for energy. Remember, you lost weight. The fat that was burned was animal fat (you are an animal). That fat was highly saturated and contributes to your high cholesterol production. Once that fat is off your body completely the picture will be different. In other words, once your weight has stabilized at this lower level, you will see an improvement in your cholesterol results, including a better LDL particle size and number.
I am a thin female, age 60, 5’ 7", weight 119-120. I eat a very strict Nutritarian diet and exercise 3-4 days per week. How much fat (percentage) is allowable and will not elevate my cholesterol level or clog my arteries? I really love nuts/seeds and avocados but just am never sure how much fat is safe. I went to a local health lecture by Dr. Caldwell Esselstyn, who states all fat is detrimental and causes damage to arterial walls. He recommends only 8-10%, but I know from reading your books that fat is necessary for brain health and heart health. I just get very confused. If I have a percentage to go by, like 20% or 25% of total calories from fat, I can better gauge how much is healthy. I tend to lose weight easily and really don’t like getting too thin.
There is no level of fat that is detrimental to the body if you are thin and utilizing the fat for energy, and it is from healthy food sources such as seeds and nuts. In fact, higher intake of seeds and nuts lower LDL cholesterol even more than lower amounts. Plus, seeds and nuts enlarge the LDL molecule (fluffy) reducing risk further, so the number does not even represent the degree of protection. Nevertheless, a small difference in cholesterol would not make much difference when every other parameter of risk improves, including less risk of arrhythmia and sudden cardiac death, as well as lower risk of cancer with the inclusion of seeds and nuts.
Did you ask the doctor making that claim to show the studies that determine that conclusion, and what type of fats were used in those studies? If you did, you would find no evidence for that conclusion. That was only from processed oil; in fact when they tried to reproduce inflammatory markers with nuts and seeds they found the opposite, that it decreased inflammation. There are more than one hundred studies documenting that nuts and seeds are favorable foods for the heart and blood vessels and none demonstrating unfavorable effects, so excluding them has no basis in science.

Julie lost 60 pounds, lowered her cholesterol, and avoided going on medication... Read More
Results may vary.
Jeff lost 35 pounds and is thankful to have his health back again; he no longer suffers from irritable bowel syndrome and lowered his cholesterol... Read More
Results may vary.
For years Tom tried to lower his cholesterol, only by following the Nutritarian diet style was he successful... Read More
Results may vary.
Steffi lost 18 pounds and with it went her constant cravings for sugar and her high cholesterol... Read More
Results may vary.
A genetic disordor caused Gloria's very high cholesterol; after stopping her meds and changing her diet for just 3 months her cholesterol is significantly lower... Read More
Results may vary.
Averill lowered his cholesterol; learned older age doesn't mean more medication and is determined not to follow his family's history of bad health... Read More
Results may vary.
Jean so quickly lowered her cholesterol that her doctor now recommends Eat To Live to patients... Read More
Results may vary.